

In the fall of 2016, proponents of legalizing medical marijuana in Arkansas touted studies suggesting that cannabis was a safer alternative to pain pills.
Voters that year approved a constitutional amendment allowing patients — with a doctor’s approval — to get and use marijuana, joining a rapidly spreading national trend. But has the promise of safer pain management been realized? Academic researchers say probably not, but it’s a question still ripe for investigation.
The Arkansas Center for Health Improvement applied in October for a $1.4 million grant from the National Institutes of Health to study the effect of medical marijuana on opioid use. “I don’t think right now we know much about what the impact of medical marijuana has been on opioids itself,” ACHI President and CEO Dr. Joe Thompson told Arkansas Business last week.
He said ACHI applied for the grant to determine whether medical marijuana has reduced the number of opioid prescriptions. “Our grant actually says it could go either way,” Thompson said. “It could be helpful or it could be harmful.”
He said he expects to learn by the middle of the summer if the grant is approved.
The state’s first medical cannabis dispensaries opened in May 2019, and since then more than $218 million worth of cannabis has been sold at 32 licensed dispensaries.
Nearly half of the 444 drug overdose deaths reported in Arkansas in 2018 involved opioids — a total of 208 fatalities, according to the latest figures from the National Institute on Drug Abuse. There were 352 drug overdose deaths in 2019, but the share of those deaths attributed to opioids was unavailable.
Arkansans, however, have been heavy users of opioids. In 2018, Arkansas physicians wrote 93.5 opioid prescriptions for every 100 people compared with the U.S. average of 51.4 prescriptions, the NIDA said. In 2019, Arkansas’ number dropped to 80.9 opioid prescriptions for every 100 people.
At Arkansas’ peak in 2014, 123 opioid prescriptions were written for every 100 people, when the national average was 75.6. Data for 2020 hasn’t been released.
Even though opioid use has been falling in Arkansas, it’s unclear if the trend is related to the availability of medical marijuana.
At New Beginnings CASA in Warren, a 32-bed inpatient rehabilitation facility, there has been a decrease in residents’ opioid use, Executive Director Mitzy Sullivan said. “I don’t know if it’s because of the medical marijuana, but being in southeast Arkansas, we see a lot of methamphetamine use.”
Since 2016, Arkansas Blue Cross & Blue Shield has seen a drop in claims for opioid prescriptions, according to Max Greenwood, vice president for government and media affairs for the state’s largest health insurance provider.
The decline in opioid use is attributed to changes that include limits on prescriptions. ABCBS also has seen increases in the use of medication to treat opioid substance abuse disorder. “Bottom line, we believe the decrease we’ve experienced is a result of our internal actions … and have no indication it has any correlation with medical marijuana laws,” Greenwood said in an email.
Medical marijuana, which in Arkansas costs some $400 an ounce on average, is not covered by insurance.
Arkansas Drug Director Kirk Lane said any reduction in opioid use so far can’t be linked to medical marijuana. But, he said, “I’m sure the medical marijuana industry would enjoy” claiming that.
In recent years, several programs have been started to reduce opioid abuse in Arkansas, including teaching providers about prescribing decisions involving opioids. “Medical marijuana really hasn’t played an issue in our prescribing rate reduction,” Lane said.
Also helping reduce opioid abuse in recent years were new prescription guidelines from the Centers for Disease Control & Prevention, said Jamie Turpin, the Prescription Drug Monitoring Program administrator at the Arkansas Department of Health.
“At the Health Department and many other entities, there are programs to help educate providers on these guidelines to promote codispensing of an opioid with Naloxone,” a medication that can counteract an opioid overdose.
Also in 2017, Arkansas passed a bill that required prescribers to check with the prescription drug monitoring program database before writing a prescription for opioids. That program helps prevent patients from hopping from one doctor to another for opioid prescriptions.
It’s difficult to say what factors have reduced the number of opioid prescriptions, said Lane.
Positive Studies
Still, there are studies that show a link between marijuana availability and a reduction in the number of opioid deaths.
A study released last month by two marketing professors found that in counties that had legal cannabis sales, an increase from one to two dispensaries was linked to an estimated 17% reduction in all opioid-related deaths between 2014 and 2018.
Arkansas, where legal cannabis was not available until mid-2019, was not included in the study.
“We’re just showing that there’s this association that should be investigated more,” said Greta Hsu, professor of management at the Graduate School of Management, University of California, Davis. She conducted the study with Balázs Kovács, associate professor at the Yale University School of Management.
“It’s difficult with this kind of study to really pinpoint causality. What you would need to do is follow individuals.”
Hsu said the study shouldn’t be fodder in arguments over states seeking to legalize marijuana.
“All we’re trying to say is, we need to think about the potential benefits for overall public health and weigh that carefully against the negatives,” Hsu said. “And so this is maybe one piece of information that we can take in and kind of piece together the bigger puzzle.”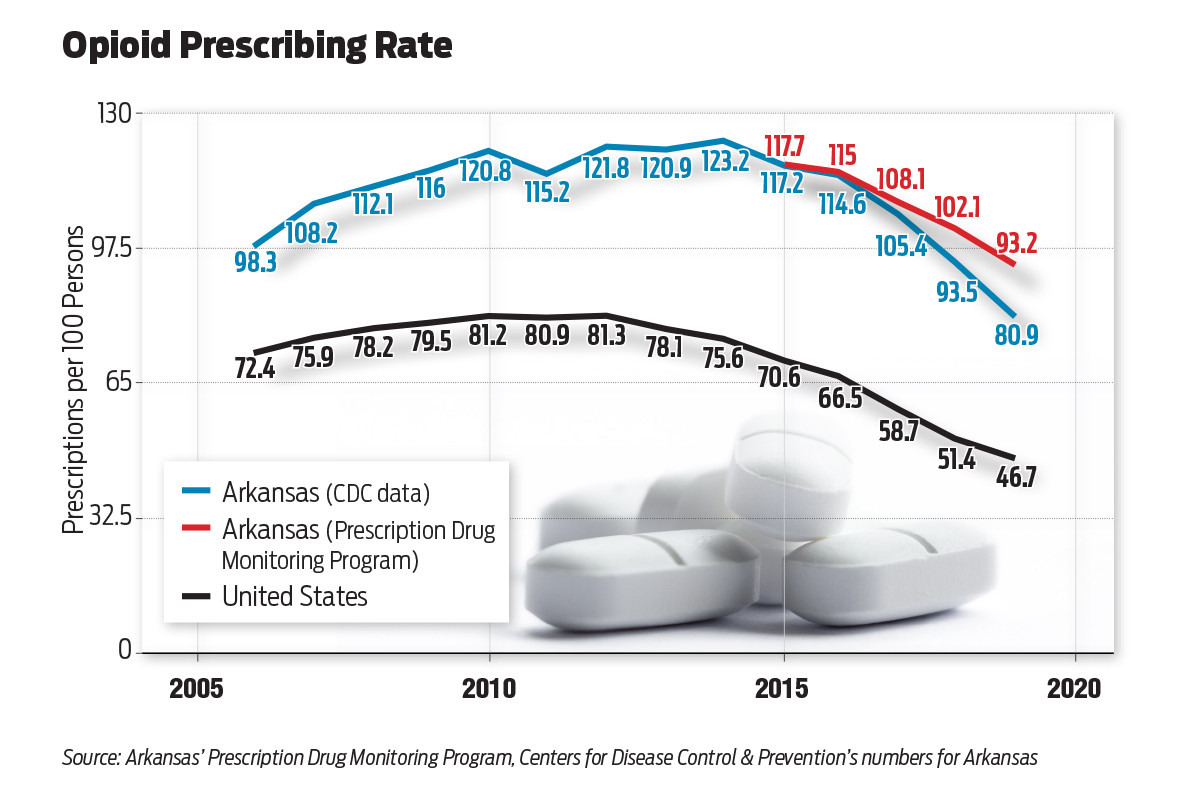
Inspiration
The prospect of providing a safer alternative to addictive painkillers has been a motivator in the medical marijuana industry. Storm Nolan, who has a license for a marijuana cultivation business to be located in Fort Smith, told Arkansas Business last year that his late mother’s opioid addiction inspired his interest.
Dispensary owner Kattie Hansen said she decided to go into the medical cannabis business after witnessing friends and relatives struggle with addiction “to the point where it destroyed them and their families,” she said.
“For so long we’d been educated that drugs are bad, that marijuana is a gateway drug, and you classify it as something harmful or dangerous,” Hansen said.
“But once I saw a really close family member go through a terrible time with opiates, I started rethinking.”
She said when she understood what marijuana could do, “I started spreading the word to family and friends.
“Now it’s really a passion of mine, and an industry that I knew I could be a part of and really bring change to people who are hurting,” Hansen said.
Hansen was an owner of a marijuana dispensary in Hensley, but sold her interest in that and received a license for a new dispensary, Native Green Wellness Center, that she and her father, Walter Koon, are preparing to open at 3720 Cantrell Road in Little Rock. (See Little Rock Tire Shop Shifts Gears to Cannabis.)
Studies have shown that the first states to decriminalize or legalize marijuana experienced a decline in prescriptions for opioids, said Chelsea Leigh Shover, an epidemiologist and health services researcher who is an assistant professor at the University of California, Los Angeles.
And initial research indicated a correlation between states with medical marijuana and a reduction in opioid deaths, she said.
“It’s a nice idea,” Shover said. “I wish it were true that if you legalize medical cannabis that reduces opioid use disorder and opioid overdose deaths.” But further studies have not proved a correlation, she said.
Keith Humphreys, a professor of psychiatry and behavioral sciences at Stanford University, agreed.
“Lots of things can be associated when you correlate things at the state level,” he said.
But there isn’t any evidence proving that medical marijuana reduced opioid use disorder or deaths. “It’s certainly been claimed as such,” Humphreys said. “But you have to remember there’s a multibillion-dollar industry that is trying to get itself established, and so making that claim helps their case. But it doesn’t mean it’s true.”
Shover said studies are mixed on whether individuals would use fewer opioids if cannabis was available. “It probably doesn’t have that effect,” Shover said.
There’s probably “some subset of the population” for which that is true, but “when you get the whole population together, that’s not what you see.”
Still, there are several policy and public health reasons for states to think about legalizing marijuana, she said.
“But the idea that just legalizing is going to meaningfully affect opioid use or opioid use disorder, that idea really isn’t supported by high-quality evidence,” Shover said.












